Gallenblase und Gallenwege
Was ist die Gallenblase und welche Funktion hat sie?
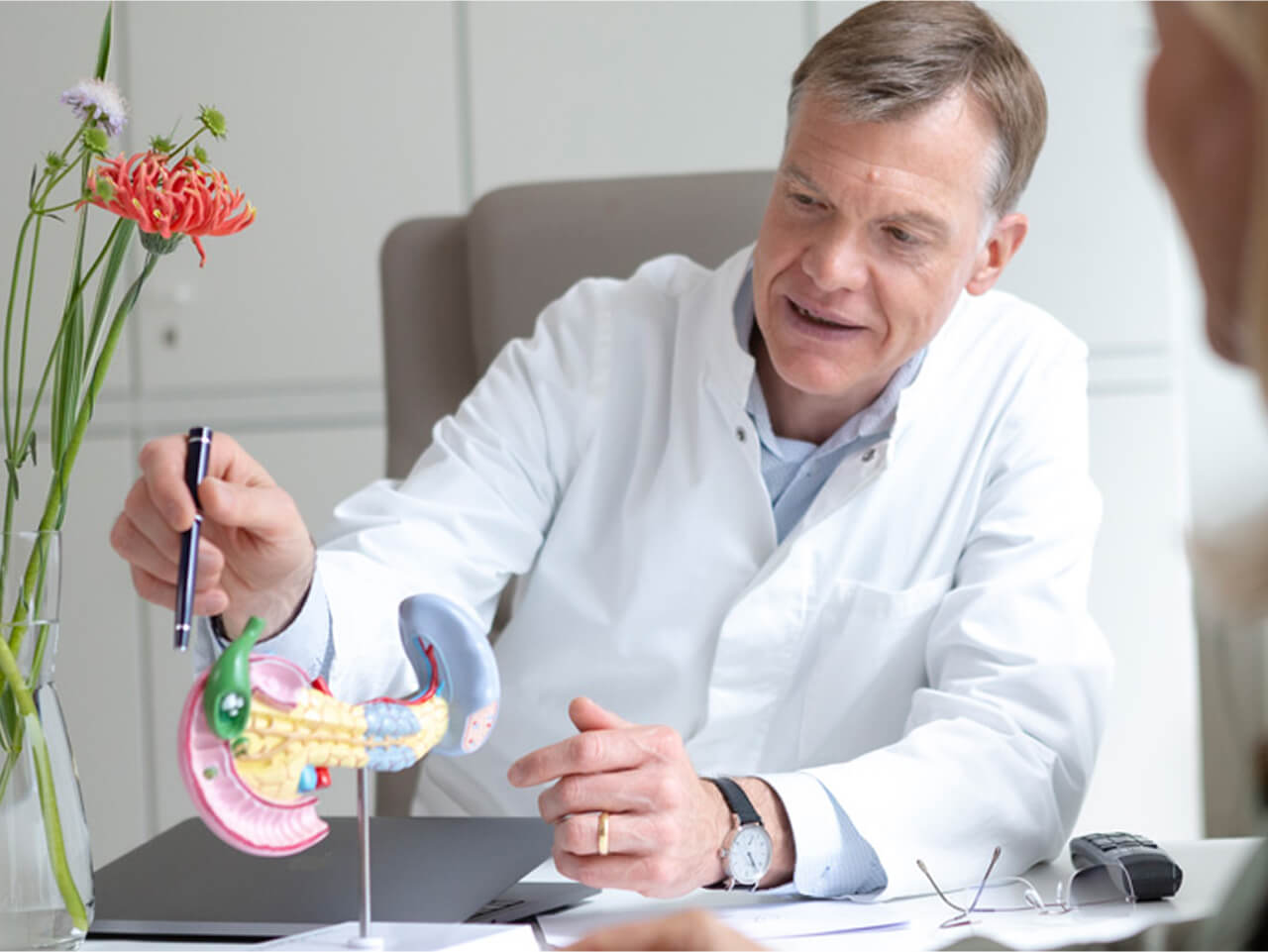
Die Gallenblase ist ein Hohlorgan unterhalb der Leber. Sie speichert die von der Leber produzierte Gallenflüssigkeit und gibt sie bei Bedarf in den Zwölffingerdarm ab, um die Verdauung von Fetten zu unterstützen. Die Gallenblase ist somit ein wichtiger Teil des Verdauungssystems.
Die Leberzellen produzieren täglich 800 bis 1000 Milliliter Galle, welche über den Gallengang in den Zwölffingerdarm fließt. Zwischen den Mahlzeiten wird ein Teil der Gallenflüssigkeit in der Gallenblase gespeichert. Sobald eine (fettreiche) Mahlzeit eingenommen wird, gibt die Gallenblase die gespeichert Menge über den Gallengang ebenfalls in den Zwölffingerdarm ab. Muss die Gallenblase aufgrund von Steinen (Cholezystolithiasis) und Entzündung (Cholezystitis) entfernt werden, fließt die Galleflüssigkeit weiterhin in den Zwölffingerdarm, die Speicherfunktion der Gallenblase fällt aber weg. Das erfordert aber keine Änderungen der Ernährung.

Für Sie da – persönlich, erfahren, verlässlich.
Eine erfolgreiche Behandlung beginnt mit einem persönlichen Gespräch.
Mittwoch von 15:30 bis 20:00 Uhr nach Voranmeldung
Weitere Termine nach Vereinbarung.
Erkrankungen der Gallenblase
Gallensteine
Zu den häufigsten Erkrankungen der Gallenblase zählen Gallensteine (Cholezystolithiasis). Sie entstehen durch Kristallisation und Ablagerung schlecht löslicher Bestandteile der Gallenflüssigkeit. Ein typisches Symptom ist die Gallenkolik, dabei blockiert ein oder mehrere Steine den Ausführungsgang der Gallenblase für eine gewisse Zeit, die Kontraktionen der Gallenblase gegen diesen Widerstand verursachen die Schmerzen. Symptomatische Steine in der Gallenblase erfordern eine Behandlung, letzlich die chirurgische Entfernung der Gallenblase zusammen mit den darin befindlichen Steinen (Cholezystektomie). Dies erfolgt meist mittels Schlüsselloch-Chirurgie (laparoskopische Cholezystektomie).
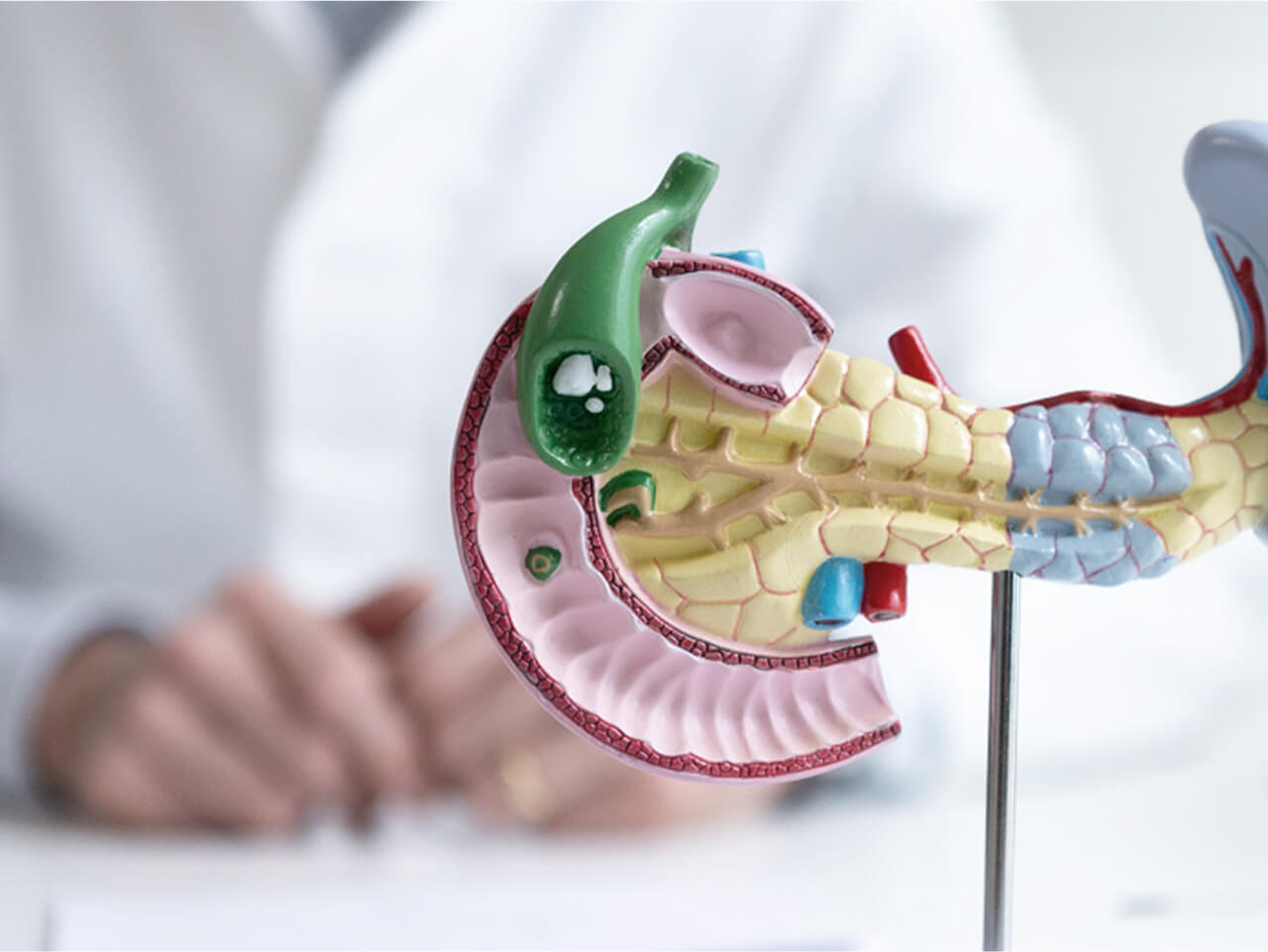
Gallenblasen- und Gallengangkrebs
Bei Gallenblasenkrebs handelt es sich um einen bösartigen Tumor in der Gallenblasenwand. Im Vergleich zu anderen Krebsarten tritt ein Gallenblasenkarzinom sehr selten auf, die Ursachen konnten bislang nicht vollständig geklärt werden. Beim Gallengangkrebs entsteht der Tumor aus den Zellen der Gallengänge. Sowohl Gallenblasen- als auch Gallengangkrebs verursachen oft über lange Zeit keine Symptome und werden meistens erst im fortgeschrittenen Stadium erkannt. Daher ist das Risiko, dass die Tumore in andere Organe streuen und Metastasen bilden, sehr hoch.

Krankhafte Veränderungen der Gallenblase und Gallenwege bedürfen einer genauen Abklärung und Behandlung. Manchmal kann auch das Wachstum eines Tumors aus der Gallenblase oder den Gallengängen Ursache von Symptomen sein, deshalb sind eine exakte Diagnose und die Unterscheidung zwischen Stein, Entzündung und Tumor unerlässlich für eine korrekte Behandlung.
Welche Symptome treten bei Erkrankungen der Gallenblase auf?
Viele Erkrankungen der Gallenblase verursachen anfangs keine Beschwerden und werden demnach auch nicht wahrgenommen. Gallensteine können zu unspezifischen Schmerzen im Oberbauch führen und ein Völle- oder Druckgefühl auslösen. Meistens treten diese Beschwerden direkt nach einer Mahlzeit auf. Plötzlich auftretende starke Schmerzen weisen auf eine Gallenkolik hin.
Viele Beschwerden, die bei Erkrankungen der Gallenblase auftreten, sind uncharakteristisch und können auch auf andere Krankheiten hindeuten. Das trifft auch auf das Gallenblasenkarzinom zu. Ein wichtiges erstes Anzeichen für Gallenblasenkrebs ist ein Gallenstau (Cholestase), der durch den Tumor verursacht wird und den Abfluss der Galle behindert. Typische Symptome dafür sind eine Gelbfärbung der Haut und des Augenweißes (Ikterus, Gelbsucht), die Braunfärbung des Urins und die Entfärbung (grau-weiß) des Stuhls.
Sollten Sie solche oder ähnliche Symptome bei sich feststellen, berate ich Sie gerne ausführlich über Diagnostik und Behandlungsmethodik.
Prävention: Wie können Probleme
mit der Gallenblase vermieden werden?
Es gibt verschiedene Möglichkeiten, das Risiko für Erkrankungen der Gallenblase zu reduzieren. Vor allem sollte auf eine ausgewogene Ernährung geachtet werden. Ballaststoffreiche, cholesterin- und fettarme Mahlzeiten, die über den Tag verteilt eingenommen werden, haben sich als beste Möglichkeit erwiesen, die Gallenblase zu entlasten und Erkrankungen vorzubeugen. Darüber hinaus ist regelmäßige Bewegung empfehlenswert und der Alkohol- sowie Nikotinkonsum sollten reduziert werden.
Ich berate Sie bei Erkrankungen der Gallenblase und der Gallenwege zur passenden Diagnostik und Behandlung.

Ihr Spezialist für Erkrankungen der Gallenblase und Gallenwege in Wien
Als Facharzt für Allgemeinchirurgie, Viszeralchirurgie mit Spezialisierung auf Erkrankungen der Gallenblase und Gallenwege biete ich eine umfassende Diagnostik, individuell abgestimmte Behandlung und persönliche Betreuung – von der Abklärung bis zur Nachsorge.
Häufig gestellte Fragen (FAQ)
Was passiert bei einer Gallenblasen-Operation?
Die Gallenblase wird samt Steinen entfernt, meist per Schlüssellochchirurgie (minimal-invasiv). Die Verdauung funktioniert auch ohne Gallenblase normal.
Muss ich nach einer Gallenblasen Operation Diät halten?
Nein. In der Regel können Sie nach der Operation normal essen. Beschwerden nach fettreichen Mahlzeiten bessern sich meist. Wichtig bleibt eine ausgewogene Ernährung.
Muss ich meine blutverdünnenden Medikamente absetzen?
Das hängt von der Medikation ab. Bitte teilen Sie mir diese mit – ich kläre ab, ob und wie sie vor einer Operation angepasst werden müssen.
Wie laufen die Untersuchungen vor einer Operation ab?
Das hängt vom Eingriff ab. Ich unterstütze Sie bei der Planung individuell notwendiger, präoperativer Untersuchungen. Bei kleinen Operationen reichen Anamnese und klinische Untersuchung. Bei großen Eingriffen oder auffälligen Befunden sind zusätzliche Untersuchungen erforderlich (z. B. Herz, Lunge, Blutgerinnung).


